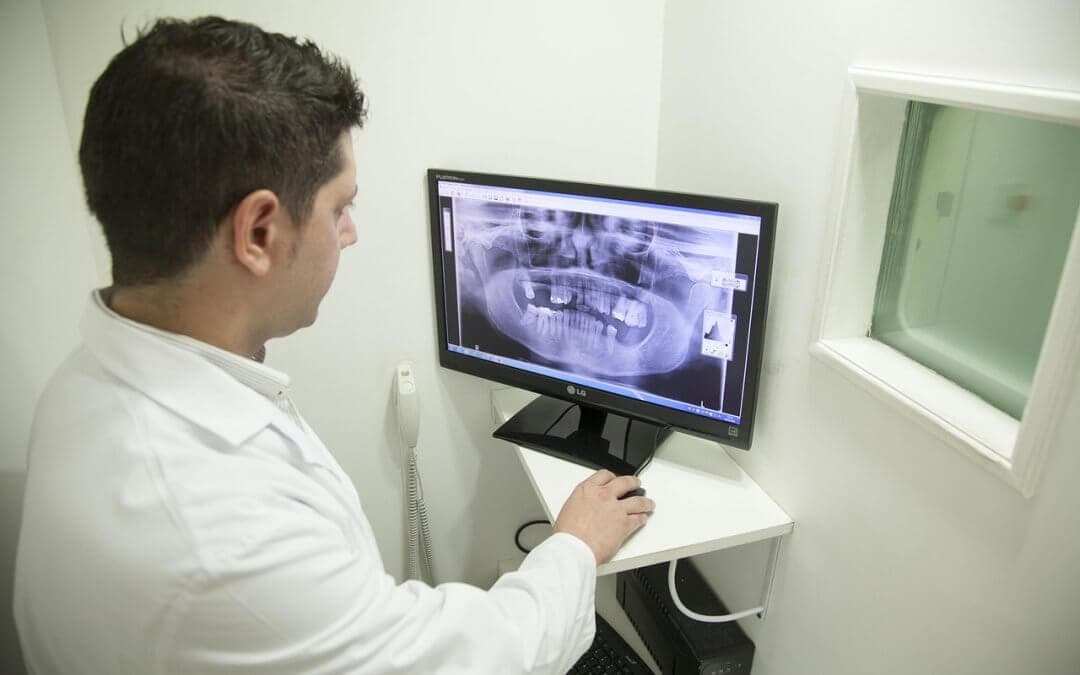
Imaging centers face pressure to move patients through scans while maintaining high standards of care and accurate results. Artificial intelligence is changing how teams schedule, scan, read and report studies, easing daily friction and shifting routine work to machines.
From queue prioritization to error detection, AI offers tools that cut wasted time and let staff focus on harder cases. The following outlines practical ways AI is streamlining operations so clinics can run smoother and patients receive faster answers.
AI Scheduling And Patient Flow
AI driven scheduling systems look at many factors at once such as modality availability, staff skills, and patient constraints to build a rhythm that keeps the day on track. These tools can predict no shows with a level of nuance that helps teams offer open slots to those most likely to attend, which reduces idle scanner time and stabilizes revenue.
Automated reminders that adapt their tone and timing based on prior behavior raise attendance rates while freeing front desk staff from repetitive calls and texts.
In busy centers, this type of automation also supports helping teams scale without extra staff while maintaining steady patient flow. When slot lengths are predicted from past exams and patient notes, throughput improves and the whole clinic begins to feel less frantic.
Automated Image Triage And Prioritization
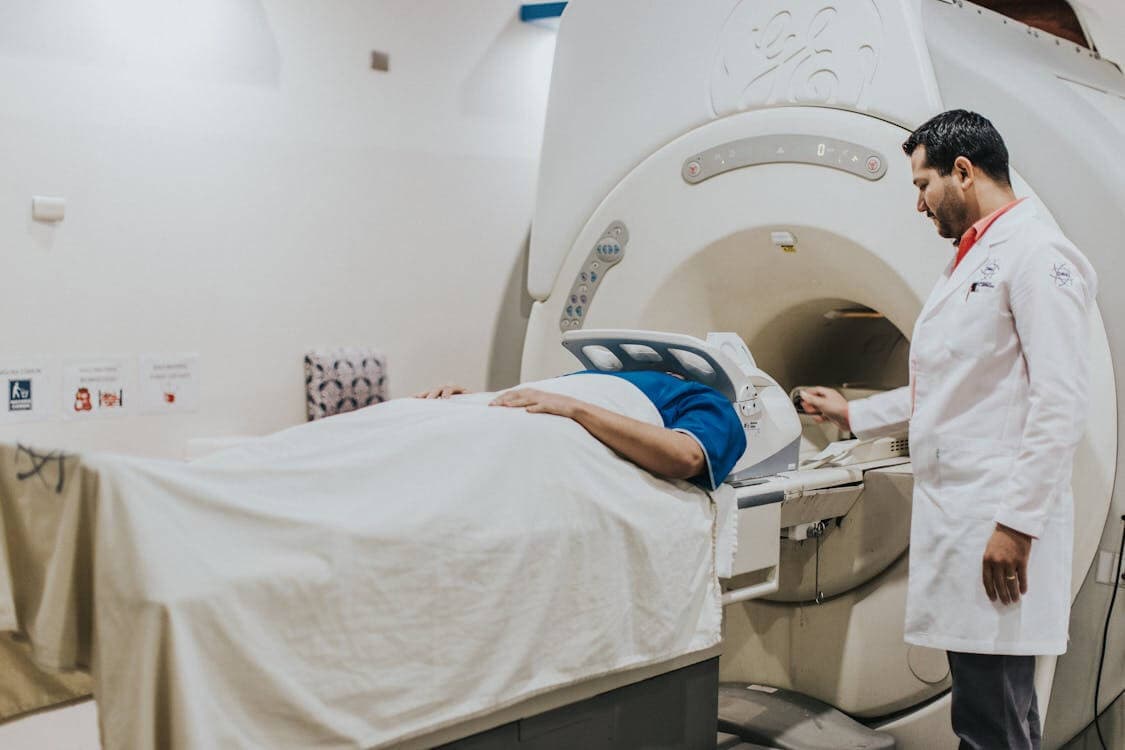
Algorithms can flag urgent findings on incoming scans and move critical cases to the front of the reading queue, creating a safety net for patients who need rapid attention. Radiologists receive an ordered workflow that places likely fractures, bleeds, or acute pathologies higher up, which means lifesaving reads are no longer a needle in a haystack.
This triage reduces time to treatment for serious cases and trims the latent burden that grows when routine cases swamp oncall work. Over time the system learns which alerts were most useful and refines thresholds so false positives do not drown staff in noise.
Intelligent Protocol Selection
Choosing the right scan protocol is a subtle task that blends clinical history, patient condition, and scanner capabilities, and AI can act like an expert second pair of eyes. When a technician uploads a brief description or when the electronic chart is queried, models suggest protocols that match clinical intent while balancing scan time and image quality.
These recommendations reduce repeat scans that occur because of suboptimal sequence choice, which improves patient comfort and cuts unnecessary dose exposure for studies that involve ionizing radiation. With fewer retakes and clearer exams, reporting becomes more efficient and confident reads happen sooner.
Workflow And Resource Optimization
AI can monitor the ebb and flow of activity across a center and recommend staff assignments, room allocations, and equipment rotation that fit the actual demand curve. Predictive models estimate peak hours and suggest where to place float techs so scans start on time and fall behind less often, which keeps the whole team moving in step.
Supply levels such as contrast media can be tracked and reordered based on usage patterns, reducing the chance of last minute scrambles that slow a day down. When mundane logistics run in the background, humans have room to focus on nuance and patient care.
Quality Control And Error Detection
Automated quality checks inspect images as soon as they leave the scanner, spotting motion artifact, wrong field of view, or missing sequences before the patient leaves the site. Alerting a technologist while the patient is still on the table gives a chance to correct an issue immediately, saving time and avoiding the hassle of a recall.
Image analysis can also compare current studies to prior exams and flag mismatches that signal a wrong patient or wrong side, which adds a layer of safety that complements human vigilance. These processes act like a watchdog that keeps standards high without wearing staff thin.
Reporting And Natural Language Assistance
Natural language models assist radiologists by drafting structured reports from findings and measurements, which can shave minutes off each read and reduce repetitive typing. These drafts reflect common phrasing and local style so edits are light touch, and they pull in prior results and key history so reports are coherent and well linked across time.
When radiologists accept or adjust suggested text, the models learn and begin to echo preferred voice and terminology, creating a feedback loop that tightens quality. Searchable, consistent reports speed consults with referring clinicians and make follow up easier.
Predictive Maintenance For Equipment
Scanners and supporting devices send a stream of status signals that AI can analyze to forecast component wear and imminent faults with surprising accuracy. Rather than waiting for a breakdown that halts scheduling, teams receive a heads up that part replacement or service will be needed, which allows planned downtime and minimal disruption.
Early intervention cuts long emergency repairs and often extends the usable life of key parts, which helps budget planning and keeps patient care steady. When machines behave predictably, staff stress drops and the clinic runs more like clockwork.
Patient Experience And Communication
AI tools personalize appointment outreach by matching message style to patient preferences and by suggesting arrival times that fit real world traffic patterns and clinic flow. Mobility needs and language preferences can be incorporated so instructions are clearer and prep errors fall away, creating a calmer experience for people who may be anxious about scans.
Virtual assistants can answer simple questions about fasting, metal implants, or contrast risks, freeing staff to address the questions that really need human judgment. Little improvements in clarity and timing tend to add up, and patients notice when their visit feels smooth and respectful.